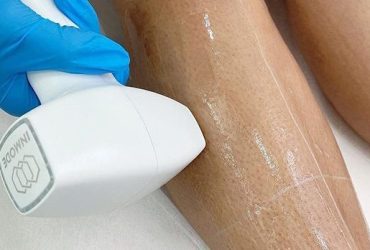
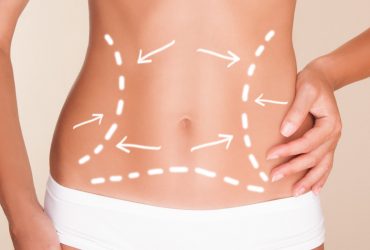
Adipocytes store energy in the form of cytosolic triglycerides. These fat cells make up adipose tissue in the body and are held together by an organized lobular network of collagenous fibrous septae. Adipocytes can distend dramatically with increased triglyceride content. Excess adipose tissue can lead to aesthetically displeasing body contour bulges and convex distensions. Fat lobules are contained within and partitioned by fibrotic septal divisions running perpendicular and oblique to the surface of the skin. In females, these partitions can weaken and the orientation of the septae be altered, resulting in focal herniations of fat into the dermis, creating the classic bulging skin nodules of cellulite [1]. Suction-assisted Lipoplasty (SAL) performed under tumescent anesthesia has long been the gold standard treatment to reduce focal fat excess [2]. Recently, ultrasound, laser, and radiofrequency (RF) technologies have been added to traditional lipoplasty, resulting in energy-based liposuction, to improve the soft tissue contraction, and minimize ecchymosis
Background and Objective:
A novel, noninvasive technology, utilizing suction-coupled radiofrequency (RF) heating and ultra-short pulse duration, high-voltage electrical pulses was studied for its efficacy and safety on adipose tissue reduction.
Methods:
Twenty-one subjects underwent treatment of their abdominal fat once weekly for 6 weeks. Clinical outcomes including abdominal circumference, adipose tissue thickness (measured by ultrasound), adipose tissue weight, body weight, and clinical photographs were obtained at visits 1 and 3 months after last treatment. Adverse events were recorded. Three subjects, who were
undergoing a future elective abdominoplasty, were treated with the same protocol, but on only one side of the abdomen before abdominoplasty. Biopsies from the RF-treated and untreated sides were harvested during abdominoplasty and cultured; measurements of adipocyte size and shape, rate of apoptosis, collagen production, and dermal thickness were determined.
Results:
Significant clinical improvements (P<0.05) were observed for the following clinical outcomes: reduction of abdominal circumference (113.4–110.7 cm), reduction of subcutaneous adipose tissue thickness (40.5–38.5 mm), and reduction in adipose tissue weight (32.2–30.7 kg) at 3-month follow-up visits. Overall patient weight also decreased, which was statistically significant at 1-month
follow-up, but was not statistically significant at 3-month follow-up (73.9–73.3 kg, P¼0.609). Histologically, adipocytes were observed to have decreased size and withered shape, with increased levels of apoptosis; increased collagen synthesis, with compaction and reorganization of the dermis was also observed. Only minor, transient side effects were reported.
Conclusions:
This novel, noninvasive RF device was effective for improving subcutaneous fat, reducing abdominal circumference and reducing subcutaneous fat layer thickness. Histologically, these improvements appear to be partly related to increased adipocyte apoptosis.
Lasers Surg. Med. 46:94–103, 2014. 2014 Wiley Periodicals, Inc.
To Download the Complete A Clinical and Biological Evaluation, click here.